Denial Management in Healthcare: How to Reduce Denials and Get Reimbursed Faster
A complete guide to denial management in healthcare. Learn how to reduce denials, improve RCM workflows, and accelerate reimbursements.
March 23, 2026


Key Takeaways:
• Most claim denials follow a predictable pattern—and because they're predictable, they're fixable with the right process in place.
• Payers communicate denial through ERAs and EOBs using CARCs and RARCs. Correctly interpreting these codes determines whether a claim needs a simple correction or a formal appeal.
• Every payer enforces strict appeal deadlines. Missing the window turns a recoverable claim into a permanent write-off.
• Claim denials fall into 5 categories: hard, soft, preventable, clinical, and administrative. Knowing the type determines how you respond and how fast you can recover the revenue.
• The IMMP framework—Identify, Manage, Monitor, Prevent—gives denial management teams a structured approach that moves from reactive firefighting to proactive prevention.
• AI-powered denial management connects prevention, detection, prioritization, and appeals in one workflow, replacing the reactive manual process most teams still rely on.
Every denied claim is revenue that doesn’t hit your books on time.
And most denials follow a very familiar pattern: a claim gets denied, your team investigates, and by then the same issue has already rippled across other claims, adding to rework before the root cause is ever fixed. This creates ongoing pressure for healthcare providers dealing with rising claim denials and delayed reimbursements.
What makes it worse is that denial rates aren’t staying flat—commercial claim denials rose 20.2%, and Medicare Advantage denials jumped 55.7% between 2022 and 2023 alone, per the American Hospital Association.
That's where effective denial management comes into the picture.
In this article, we'll break down what denial management in healthcare involves, how denials are identified and prioritized, and how AI is helping RCM teams build systems that resolve them faster and strengthen healthcare denial management in RCM.
What is Denial Management in Healthcare?
Denial management in healthcare is the process of identifying, analyzing, and resolving claims that have been denied by payers, while also addressing the underlying issues that caused those denials in the first place.
When a payer refuses to reimburse a provider for a service rendered (whether fully or partially), that’s a denial. Denial management is everything that follows: figuring out why it happened, fixing it, appealing it where possible, and making sure it doesn’t happen again.
In hindsight, it looks like a backend function. But effective claims denial management in healthcare works both reactively and proactively:
- Denial resolution (reactive): Involves working on denied claims after they occur, where the denial management team reviews denial codes, correcting errors, and resubmitting or appealing claims.
- Denial prevention: (proactive): Focuses on identifying denial patterns and fixing issues before submission, such as improving documentation, validating coding, reducing coding errors, and ensuring eligibility and authorization.
When both sides of the equation are managed well, organizations see measurably lower AR days, fewer write-offs, and faster reimbursements.
Recommended reading: Common AR scenarios in healthcare
How Do Payers Send Denials?
Payers communicate their claim decisions through an Electronic Remittance Advice (ERA) or Explanation of Benefits (EOB).
When a payer denies a claim, they include specific denial codes on these documents to explain their reasoning. It typically contains:
- Claim Adjustment Reason Codes (CARCs) to communicate the broad financial reason for the adjustment or denial.
- Remittance Advice Remark Codes (RARCs) to provide a more granular explanation of the specific issue requiring attention, if required.
Billing teams must decipher these standardized messages to determine if a claim requires a simple correction, resubmission, or a formal medical necessity appeal.
Failing to interpret the ERA correctly can lead to incorrect resubmissions, repeated claim denials, and further payment delays.
Is There a Time Limit for Filing Appeals for a Denied Claim?
Yes, every payer enforces a strict time limit for appeals. The deadlines vary significantly depending on the insurance company, the type of plan, and state regulations.
The table below is a quick reference for claim appeal time limits by payer type:
Note: The 120-day limit applies to Medicare redetermination (Level 1). Each subsequent appeal level carries its own deadline.
Missing an appeal window can turn a recoverable claim into a permanent write-off.
The numbers themselves make the case for urgency: in Medicare Advantage alone, just 11.5% of denied requests were appealed in 2024, yet over 80% of those appeals were overturned.
This shows that most denied claims have a strong chance of recovery, but only if your team acts within the deadline.
Regardless of the payer, a strong appeal must include:
- The original claim and denial notice
- The specific CARC and RARC codes cited in the denial
- Supporting clinical documentation justifying the service
- A written appeal letter addressing the exact reason for the denial
- Any relevant payer policy or LCD citations that support medical necessity
Recommended reading: How to appeal an insurance claim denial
What Are the Common Types of Claim Denials in Healthcare?
Claim denials in healthcare fall into five categories:
1. Hard Denials
Hard denials are irreversible claim rejections that result in lost revenue or patient write-offs. You cannot appeal these decisions in most cases, making them the most financially damaging type of denial.
Common triggers for hard denials include:
- Submitting a claim past the payer's timely filing limit
- Billing for a non-covered service or excluded benefit
- Providing services to a patient with terminated coverage
Since you cannot fight a hard denial after the fact, your only defense is strict front-end prevention.
2. Soft Denial
Soft denials are temporary roadblocks that can be fixed. The payer denied the claim, but they will process the payment once the billing team corrects the error(s).
Common reasons for soft denials include:
- Missing or incorrect coding modifiers
- Typographical errors in patient demographic data
- Unspecified or truncated ICD-10 codes
The medical billing staff can usually resolve soft denials by submitting a corrected claim. Prompt fixing ensures your cash flow remains steady without requiring lengthy appeal letters.
3. Preventable Denials
Preventable denials are errors that should never have occurred in the first place. They reflect gaps in internal processes that allowed an avoidable mistake to slip through.
Common triggers for preventable denials include:
- Missing prior authorization
- Eligibility not verified before service
- Incorrect coding or failure to follow payer-specific rules
Since these denials are avoidable, they represent the biggest opportunity for improvement. Identifying and fixing these patterns can significantly reduce denial volume over time.
4. Clinical Denials
Clinical denials occur when a payer determines that a service is not medically necessary or not adequately supported by documentation.
A payer will issue a clinical denial due to:
- Insufficient clinical documentation
- Diagnosis not supporting the billed procedure
- Failure to meet payer-specific medical necessity criteria
These denials require strong clinical justification and well-documented appeals, with direct provider-to-reviewer communication often being the deciding factor in overturning them.
5. Administrative Denials
Administrative denials are a result of process or data-related issues rather than clinical decisions. They often indicate breakdowns in front-end or billing workflows.
Common administrative errors include:
- Incorrect patient or insurance information
- Missing or invalid policy details
- Errors during claim submission or data entry
These denials highlight gaps in operational workflows. Strengthening intake, verification, and medical billing workflows can significantly reduce their occurrence.
While these denial types are distinct, preventable, administrative, and clinical denials often overlap in practice. At a broader level, all denial types ultimately fall under two core categories: hard denials and soft denials.
How Should You Prioritize Denials?
Not every denial deserves the same level of urgency—and treating them all equally is one of the fastest ways to burn through the team's bandwidth without meaningful recovery.
The reality is that most RCM teams are working with finite capacity. A structured prioritization system is what determines how much revenue you actually get versus how much gets written off.
1. Start with Dollar Value and Claim age
Work the highest dollar claims approaching their appeal deadline first. A $15,000 claim with 10 days left on the appeal window takes priority over a $200 claim filed recently. Dollar value and days outstanding are the primary triage lenses.
2. Factor in Payer and Denial Type
Some payers have higher overturn rates on appeal than others. Some denial types are faster to resolve than others. Knowing your historical recovery rate by payer and by denial code tells you where your team's time is best spent.
3. Separate What’s Recoverable and What Isn’t
Not every denied claim is worth working on. Categorize denials by whether they're correctable and appealable. Hard denials with no appeal pathway should be written off quickly so the team's bandwidth goes toward revenue that can actually be recovered.
4. Use Data to Build a Denial Priority Score
The most effective denial management teams go beyond manual triage. They use real-time analytics to score each denial based on dollar amount, claim age, payer, denial type, and likelihood of successful appeal—and work the list in that order.
Despite knowing these factors, most teams struggle to apply them at scale due to the manual effort required to surface these insights.
This is where a data-driven view becomes critical.
How AI Helps You Prioritize Denials
AI Agents like CombineHealth’s Taylor (AI RCM Analyst) bring all of these signals into a single dashboard—helping teams identify high-priority denials, track patterns across payers and providers, and make faster, more informed decisions on what to work next.
Taylor surfaces:
- Total denied claims and total money denied at a glance
- Denial percentage across your full claim volume
- Monthly denial rate trend—so you can see immediately whether your denial rate is improving or worsening
- Denial by payer—which payers are denying the most claims and the most dollars
- Denial by provider—which providers or departments are generating the highest denial volumes
- Denial breakdown by financial class (Commercial, Medicaid, Medicare)
- Top denial codes by frequency and dollar value
Instead of building this picture from aging reports and manual exports, Taylor puts it in front of you in real time, so prioritization decisions are based on real-time data.
.png)
What Does the Denial Management Process Look Like in Healthcare RCM?
Denial management is a continuous process that spans the entire healthcare revenue cycle. But without structure, it often becomes reactive, fragmented, and difficult to scale.
A more effective way to approach it is through a structured framework like IMMP:

This denial management framework breaks into clear stages, making it easier to move from reactive fixes to a more system-driven approach.
Identify
Determine the exact cause of each denial by analyzing Claim Adjustment Reason Codes (CARCs) and remittance advice. The goal is to pinpoint where the breakdown occurred so the issue can be corrected effectively.
Manage
Take corrective action on the denied claim—fixing errors, gathering supporting documentation, and either correcting and resubmitting or filing a formal appeal within the payer's deadline.
Monitor
Track denials by type, date, payer, and dollar value to identify patterns. Monitoring helps the team stay ahead of appeal deadlines and evaluate whether your denial management strategies are working.
Prevent
Use insights from the monitoring phase to fix root causes upstream—through staff training, updated documentation policies, and stronger front-end processes like eligibility verification and pre-submission audits.
Why Manual Denial Management Hits a Wall
Managing all four steps manually, across high claim volumes, multiple payers (and thereby multiple policies to keep up with), and constantly shifting deadlines, is incredibly hard. Most teams hit a wall here.
According to MGMA, 92% of medical group practices have had to hire or reassign staff just to manage the volume of prior authorization requests alone—a signal of how much manual effort the denial management process demands across the board.
That's exactly where AI comes in.
How AI Agents Fit Into the Denial Management in Healthcare RCM
CombineHealth's AI denials management solution connects multiple AI agents that work together as a coordinated team. Each agent handles a specific part of claims denial management in healthcare, following the IMMP framework:
- Adam (AI Denial Management Solution) navigates payer portals for claim status, makes AI-driven calls to retrieve updates, intelligently prioritizes denials by age, dollar value, and payer, and recommends next steps for resolution.
- Rachel (AI Appeals Management Solution) drafts payer-specific appeal letters in minutes, adapts to your organization's writing style, and monitors filing deadlines across all open appeals.
- Penny (AI Policy Review Solution) searches across CMS manuals and payer policies, provides precise answers with page-level citations, and flags claims at risk of non-compliance before submission.
- Amy (AI Medical Coding Solution) audits coding and documentation gaps, identifies undercoded and missing services, and ensures payer-specific coding compliance.
- Mark (AI Medical Billing Management Solution) automates claim generation and validation within medical billing workflows, navigates 50+ payer portals for eligibility verification, and identifies billing discrepancies before submission.
- Taylor (AI Revenue Cycle Management Solution) analyses each step of the RCM process, identifies bottlenecks, and streams real-time denial dashboards and performance insights.
These agents don't work in isolation. They work together like a team for a faster, more accurate denial resolution.
For example, when Adam identifies a denial, he can consult Penny for policy clarification, pull coding validation from Amy, or trigger Rachel to generate a payer-specific appeal.
.png)
Build an End-to-End Denial Management Process That Works
Every denied claim is revenue your organization has already earned.
The difference between teams that recover it consistently and those that don't comes down to having a system that identifies, monitors, manages, and prevents denials before they compound.
CombineHealth's AI agents work together across your entire denial management workflow, from catching coding gaps before submission to drafting appeals before deadlines close.
Book a demo with us to see these AI agents in action!
FAQs
1. What is denial management in healthcare?
Denial management in healthcare is the process of identifying, analyzing, and resolving claims denied by payers, while addressing the underlying issues that caused those denials.
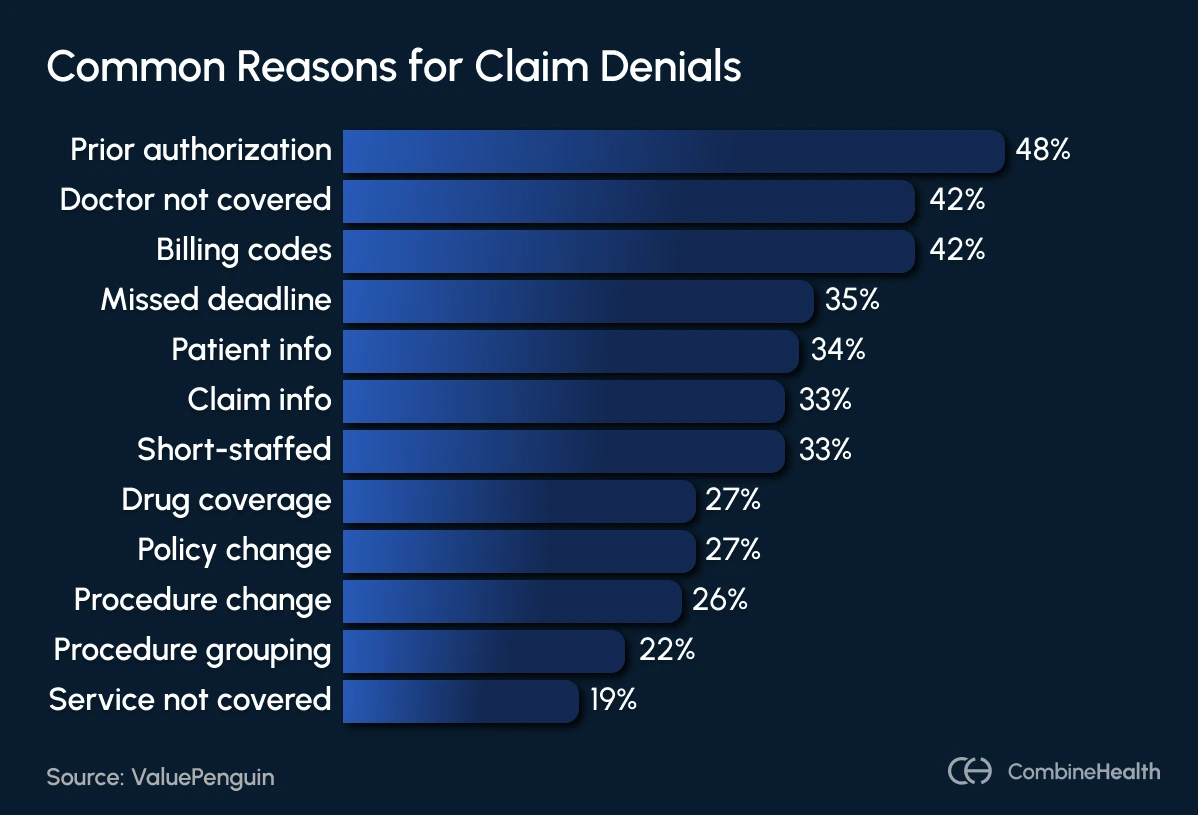
2. What are the most common reasons for claim denials?
The most common causes include coding errors, missing or expired authorizations, eligibility issues, incomplete documentation, duplicate claims, and timely filing violations.
3. How long do I have to appeal a denied claim?
It depends on the payer. Medicare allows 120 days from the date of initial determination. Medicaid varies by state, typically 30 to 90 days. Commercial payers range from 60 to 180 days, depending on the contract.
4. What is automated denial management in healthcare?
Automated denial management uses AI to handle the most time-consuming parts of the denial process—claim status monitoring, denial classification, appeal drafting, and deadline tracking—so RCM teams can focus on complex cases that require human judgment.
5. What are the best practices for claims denial management in healthcare?
Effective denial management in healthcare RCM should address both reactive and proactive sides of the process, resolving denied claims quickly while using denial data to fix root causes upstream.






