Medical Billing vs Revenue Cycle Management: A Complete Overview
Medical billing is one part of the revenue cycle, focused on claims and payments, while RCM covers the entire financial journey from scheduling to final reimbursement.
April 22, 2026


Key Takeaways:
• Medical billing is one stage within the revenue cycle. It covers charge capture, claim submission, payment posting, and patient billing, not the full financial lifecycle.
• Revenue cycle management spans every step from patient scheduling to final payment, across multiple departments and roles.
• Billing is reactive by nature. RCM is designed to catch problems before they become denials.
• Billers and RCM teams measure success differently: billing tracks clean claim rates; RCM tracks AR days, denial rates, and net collection rate.
If you're new to medical billing, chances are you've already heard the term "revenue cycle management" and assumed it was just another way of saying what you do. It's not.
Medical billing and RCM describe two different levels of the same financial process in healthcare. One is a concentrated set of tasks. The other is the end-to-end system, where those tasks live.
Knowing the difference between medical billing and revenue cycle management makes you better at the job and helps you make sense of the work happening around you.
This article breaks down exactly where billing fits in the revenue cycle and how the two processes compare.
Medical Billing vs Revenue Cycle Management: The Core Differences
Medical billing covers the mid-cycle tasks—coding, claim submission, payment posting, and patient billing. On the other hand, revenue cycle management spans the entire financial lifecycle, from the first patient interaction through final payment collection.
The cleanest way to see the divide is to compare them across five dimensions that define any operational function:
- Scope
- Ownership
- Tools
- Metrics, and
- Focus
1. Scope: Where Each Process Sits in the Cycle
While medical billing is a concentrated set of tasks, revenue cycle management is the end-to-end workflow that those tasks live inside.
RCM starts the moment a patient schedules an appointment—long before any service is rendered—and doesn't close until the final dollar is posted, whether from the payer, the patient, or both.
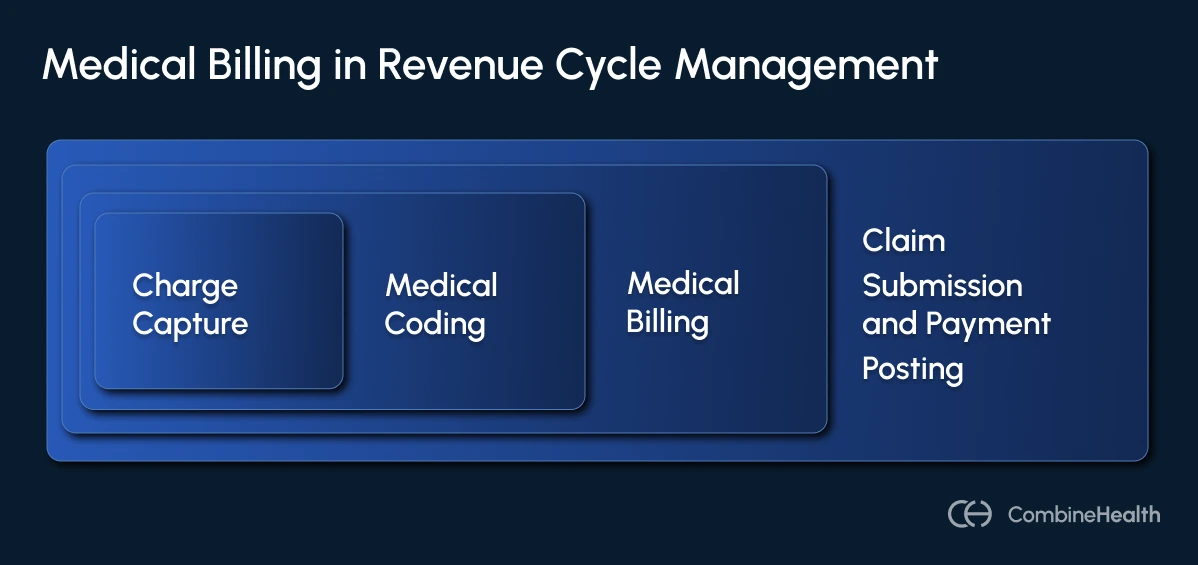
Most healthcare organizations break the full billing and reimbursement cycle into three phases: front-end, mid-cycle, and back-end.
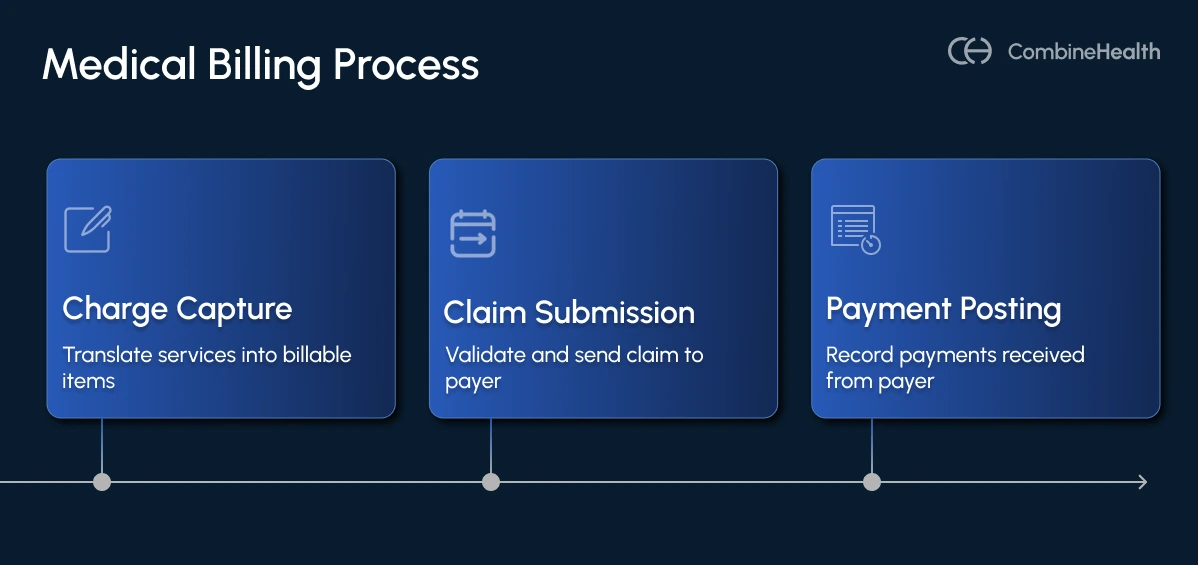
Medical billing sits in the mid-cycle and back-end of that structure. It primarily covers:
- Charge capture (translating services into billable items)
- Claim scrubbing and submission (validating and sending the claim to the payer)
- Payment posting (recording what comes back), and
- Patient billing (statements and collections for the patient's portion).
Everything in the front-end (scheduling, insurance verification, and financial counseling) happens before a biller touches a claim. The broader back-end work (denial management strategy, financial reporting, and analytics) is where RCM extends well beyond billing's reach.
2. Ownership: Who Owns the Work
A medical billing specialist owns the billing workflow. Their day revolves around claims, which involve submitting them, tracking their status, working denial queues, posting EOBs (Explanations of Benefits), sending patient statements, and communicating with payers on outstanding balances.
An RCM manager's scope is cross-departmental, and they oversee the full revenue cycle workflow, including billing. They monitor KPIs like days in AR and denial rate trends, manage the billing and coding team, review payer contract performance, identify bottlenecks at the front desk, and report financial health to leadership.
A medical biller ensures every individual's claim is processed. An RCM manager manages the system through which those claims move.
3. Tools: What Each Function Actually Uses
Medical billing runs on billing software platforms that handle claim creation, error scrubbing, clearinghouse routing, status tracking, and payment posting. This includes 2 types of billing tools:
- A billing software or a clearinghouse, from where claims are submitted to the payers, EOBs/ERAs are received, and payments are posted.
- An AI medical billing automation solution (like CombineHealth’s Mark) that performs eligibility checks, enters charges directly into the billing software, and even posts payments and reconciles totals.
Some practices outsource this entirely to a medical billing service, where a third-party vendor manages claims submission and follow-up on their behalf. However, many turn to autonomous AI medical billing platforms to do all that at a larger scale and high speed.
RCM platforms manage billing and layer in everything surrounding it. This involves RCM processes, such as eligibility verification, prior authorization tracking, denial analytics, AR aging dashboards, payer performance reporting, and patient collections.
In essence, billing software alone tells a practice whether a claim was paid. An RCM platform tells them why denials happen, where in the cycle they originate, and how to stop them from recurring.
Recommended reading: Top 22 Healthcare RCM Solutions in 2026
4. Metrics: How Each Process Is Measured
Billing and RCM teams track different numbers because they're solving different problems.
Medical billing success metrics:
- Clean claim rate: the percentage of claims accepted on first submission. HFMA sets 98% as the top-performer benchmark, with 95% as the minimum for a well-run billing operation
- First-pass acceptance rate: similar to clean claim rate; measures how often claims go through without rejection
- Days to payment: how long it takes from claim submission to reimbursement
- Denial rate by payer: tracking which payers are rejecting most frequently
RCM success metrics:
- Days in AR: the average number of days outstanding payments sit uncollected (benchmark: under 30 to 40 days, as per HFMA)
- Net collection rate: the percentage of collectible revenue actually collected after write-offs
- Denial rate: total claims denied as a percentage of total claims submitted
- Cost-to-collect: administrative cost per dollar of revenue collected
AR aging buckets: how much outstanding revenue sits in 0–30, 31–60, 61–90, and 90+ day buckets
Recommended reading: 8 Essential revenue cycle management metrics
5. Focus: How Problems Get Handled
Medical billing is, by nature, reactive. Once a claim gets submitted and is rejected,the biller investigates the denial code, corrects the error, and resubmits. The problem is addressed after it occurs.
RCM is designed to be proactive. The goal is to catch issues before they become denials.
- Eligibility is verified before the appointment.
- Authorization is secured before the procedure.
- Documentation gaps are flagged before the claim is built.
- Charge capture is reviewed before submission.
Every upstream intervention reduces the downstream rework that lands on the biller's desk.
This is the biggest operational divide between revenue cycle management and medical billing. One fixes what's broken. The other keeps it from breaking.
Medical Billing vs RCM at a Glance
Medical Billing Software vs Billing Service vs RCM Platform
These are often used interchangeably, but they’re not the same—and knowing the difference helps you understand what kind of organization you're working in and what tools you'll be using.
Medical billing software is a tool. It automates the claims management and billing workflow—building claims, scrubbing for errors, routing through a clearinghouse, tracking status, and posting payments. The biller still does the work; the software makes it faster and more accurate.
A medical billing service is a vendor. They take on the billing function on behalf of a provider, typically charging a percentage of collections. They use their own billing software and staff. What you get is execution—not strategy or upstream RCM oversight.
An RCM platform is an end-to-end system. It connects the billing and reimbursement cycle to everything surrounding it: patient access, clinical documentation, payer management, and financial analytics. The goal isn't just faster claims—it's a healthier revenue cycle overall.
Most small-to-mid-sized practices start with billing software or a billing service. As claim volume grows and denial complexity increases, the gaps in a billing-only approach become expensive—and the shift to a full RCM strategy becomes necessary.
How Modern AI Is Reshaping Billing and RCM
The biggest shift happening across billing and RCM right now is the automation wave. AI tools are taking over the repetitive, rule-based work that used to consume most of a billing team's day.
On the billing side, CombineHealth's Mark (AI medical billing solution) applies payer-specific billing rules, prepares claim-ready charges, navigates payer portals for eligibility checks, and reads ERAs and EOBs to post payments, including scanned PDF EOBs. The claim-level work that once took hours gets handled in the background, with exceptions flagged for human review.
Across the full revenue cycle, the CombineHealth AI workforce covers every stage:
- Amy (AI medical coding solution) reads encounter notes, assigns CPT, ICD-10, and E/M codes, flags documentation gaps, and provides a line-by-line rationale for every code
- Mark (AI medical billing solution) applies payer rules, builds clean claims, and manages submission and payment posting
- Adam (AI denial management solution) analyzes denied claims, navigates payer portals, places AI-driven calls to payers, and compiles appeal strategies
- Penny (AI medical policy review solution) monitors CMS and payer policies continuously, feeding updated rules back into coding and billing logic in real time
- Rachel (AI appeals management solution) drafts payer-specific appeal letters using Amy's coding rationale and Penny's policy citations
- Taylor (AI revenue cycle analytics solution) surfaces denial trends, AR bottlenecks, and revenue patterns through real-time dashboards
This is what end-to-end RCM automation looks like—a connected system where every stage feeds the next.
Connect Your Claims to the Bigger Picture!
Medical billing and revenue cycle management are two parts of the same financial engine, operating at different levels of scope.
Medical billers' work sits at the center of that engine. Every clean claim you submit, every denial you resolve, every payment you post keeps the revenue cycle moving.
But understanding where your work fits in the bigger picture changes how you approach it. The billers who grow fastest are connecting the dots between their denial queue and the upstream decisions that created it.
That's exactly what CombineHealth is built for. Mark handles the billing layer with precision. The full AI workforce covers everything around it. Book a demo to see Mark and the complete revenue cycle in action!
FAQs
1. Is medical billing part of revenue cycle management?
Yes. Medical billing covers charge capture, claim submission, payment posting, and patient billing. It's one stage within the broader RCM workflow, not a separate process.
2. Why do denials happen even when the billing team submits the claim correctly?
Because roughly denials could originate from front-end errors too, such as missed eligibility checks, missing authorizations, and bad demographics that happen before billing ever touches the case.
3. What's the difference between a medical billing service and an RCM platform?
A billing service handles claim submission and follow-up. An RCM platform connects billing to every surrounding stage—eligibility, prior auth, denial analytics, and patient collections.






