Top 5 AI Denial Analytics Vendors for Hospitals and Health Systems in 2026
Discover the top AI denial analytics vendors hospitals are seriously evaluating in 2026 to identify denial root causes, reduce claim denials, and improve revenue cycle performance.
March 11, 2026


Key Takeaways:
• Claim denials are rising and becoming a major financial burden.
• Hospitals are shifting from reactive appeals to root-cause denial analytics. Instead of working denials one-by-one, organizations analyze denial data to identify workflow gaps and prevent recurring issues.
• AI denial analytics tools help uncover patterns across payers, providers, and services. These platforms automatically categorize denials, surface trends, and highlight the operational issues driving revenue leakage.
• Leading solutions combine analytics with workflow automation. Vendors like CombineHealth, CentraMed, Imagine, Rivet Health, and Experian offer tools that improve denial visibility, prioritization, and follow-up.
• The most effective platforms connect denial insights with end-to-end RCM workflows. This allows healthcare organizations to move beyond reporting and actively reduce denial rates across the revenue cycle.
Claim denials aren’t new in healthcare revenue cycle management. But over the past few years, they’ve quietly turned into one of the biggest financial pressures hospitals face.
A 2024 HFMA report found that 82% of health system CFOs say payer denials are higher than pre-pandemic levels. At the same time, administrative complexity across the revenue cycle continues to climb. According to the American Hospital Association, more than 40% of total hospital expenses are now administrative, with prior authorizations, claims management, and denial work consuming a significant share of that cost.
Meanwhile, many health systems are realizing that appealing denials one claim at a time doesn’t solve the underlying problem. What matters more is understanding why denials are happening in the first place.
That’s why denial management is becoming a strategic priority for hospital finance leaders. This shift is also driving interest in AI-powered denial analytics platforms. By automatically categorizing denials, identifying root causes, and surfacing high-impact patterns in revenue cycle data, these tools help hospitals move from reactive denial management toward prevention.
In this guide, we’ll look at five leading AI denial analytics vendors hospitals and health systems are evaluating in 2026, and what makes each platform stand out.
What is AI Denial Analytics?
AI denial analytics refers to the use of artificial intelligence to analyze healthcare claim denials and uncover the underlying operational or documentation issues causing them. Instead of reviewing denials one claim at a time, these systems examine large volumes of claims and remittance data to identify patterns across payers, service lines, and workflows.
How Do Healthcare Practices Manage Denials with Root Cause Analytics?
Many hospitals are shifting to a proactive denial management model: root-cause denial analytics. Instead of asking, “How do we appeal this claim?”, this model allows revenue cycle teams to uncover insights like:
- Why did this denial happen?
- Where in the workflow did it originate?
- How do we prevent it from happening again?
Here’s how most hospitals operationalize denial root cause analytics.
Aggregate and Normalize Denial Data
Hospitals typically pull data from EHR, billing platforms, clearinghouses, ERAs, etc and consolidate that data into a single analytics environment to analyze:
- Denial volumes
- Denied dollars
- Denial reasons
- Payer trends
Standardize Denial Categories and Root Causes
Upon receiving an ERA/EOB from payers, hospitals map the RARC, CARC, and proprietary payer denial codes into standardized denial categories, such as:
- Eligibility or registration errors
- Missing or incomplete information
- Coding errors
- Prior authorization issues
- Medical necessity denials
- Duplicate claims
- Timely filing violations
Once denial data is standardized, analytics tools help teams identify patterns.
Conduct Cross-Functional Root Cause Reviews
Most denial issues trace back to workflow gaps across the revenue cycle, including:
- Front-end processes (registration, eligibility, authorization)
- Mid-cycle functions (clinical documentation, coding)
- Back-end workflows (billing, claim edits, payer rules)
To address this, organizations conduct cross-functional denial review meetings to review high-volume or high-dollar denial categories and determine the underlying operational issue.
Implement Denial Prevention Changes
Once root causes are identified, organizations implement operational changes designed to prevent future denials. They also continuously monitor performance using real-time dashboards and alerts that track:
- Denial rate trends
- Denial write-offs
- Appeal success rates
- Payer-specific denial patterns
- Service line performance
Best AI Denial Management Analytics Solutions
1. CombineHealth’s Taylor: Best AI Denial Analytics Solution for Mid & Large Hospitals
Taylor is CombineHealth’s AI analytics layer designed to help healthcare organizations understand what’s happening across their entire revenue cycle — including where denials originate and why they keep recurring.
The AI denial analytics platform tracks both process metrics (such as claims submitted or A/R follow-ups completed) and financial outcomes (such as net collection rate and average days in A/R), helping revenue cycle leaders identify bottlenecks that slow down reimbursements.
.png)
Taylor also provides a dedicated denials dashboard, giving revenue cycle leaders a complete view of denial performance across the organization.
The dashboard typically shows:
- Overall denial percentage
- Denials by payer (which insurers generate the most denials)
- Denials by provider
- Monthly denial trends
- Top denial categories and financial impact
Case Study: Health Center Identifies 250+ False Denials and Achieves 97.4% Accuracy Across 3,649 Claims
In one deployment at a federally qualified health center processing thousands of claims each month, Taylor helped the organization gain visibility into denial patterns that were previously buried inside EOBs.
By automatically reading and categorizing denial data, the platform achieved 97.4% accuracy in identifying and mapping denials, while also uncovering hundreds of claims that had been incorrectly classified as denied.
Read the complete case study
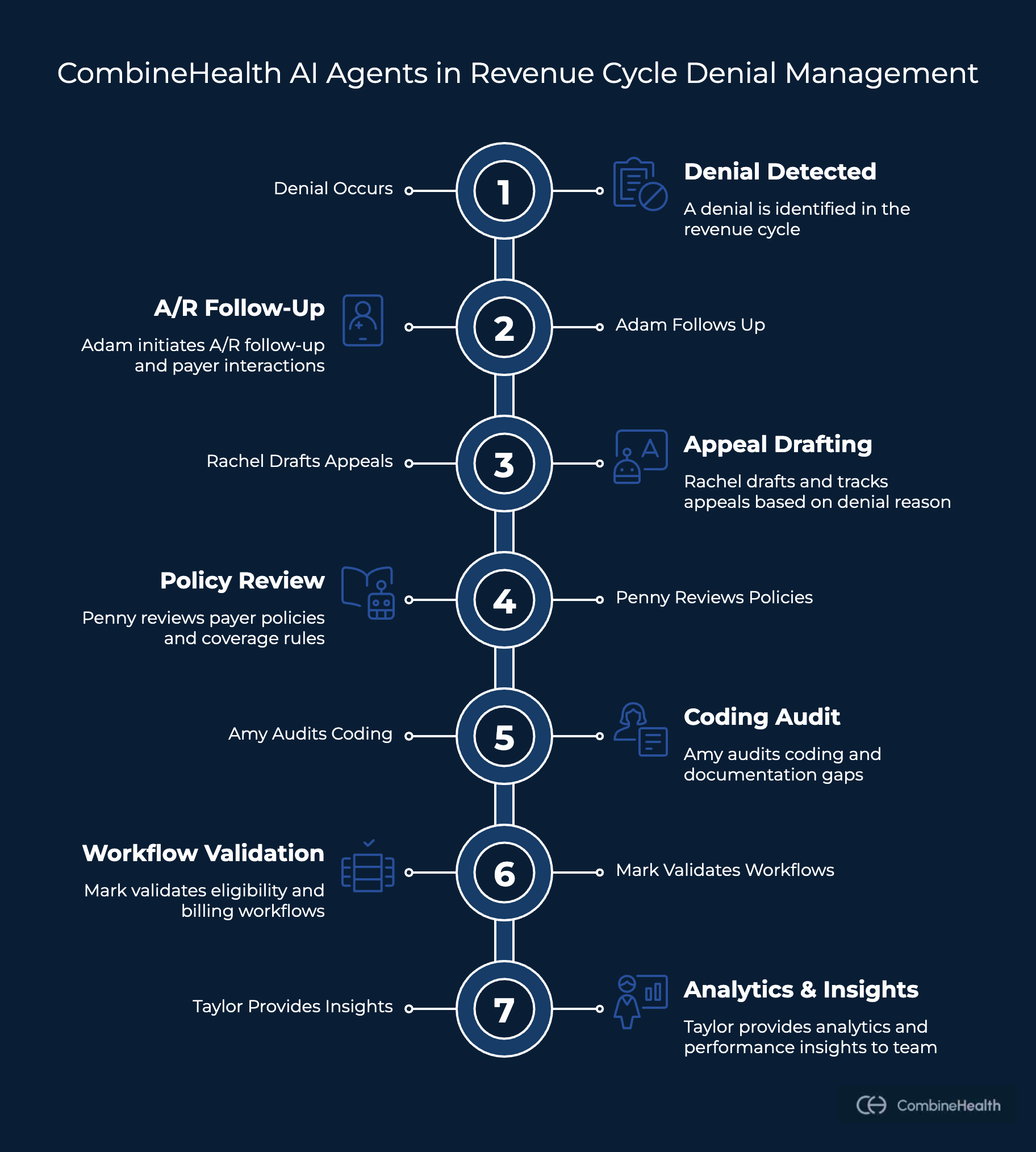
Besides denial analytics, CombineHealth offers a complete Denial Management Suite connecting multiple AI agents across the revenue cycle to prevent and resolve denials proactively:
- Adam: Manages A/R follow-up and payer interactions
- Rachel: Drafts and tracks appeals
- Penny: Reviews payer policies and coverage rules
- Amy: Audits coding and documentation gaps
- Mark: Validates eligibility and billing workflows
- Taylor: Provides analytics and performance insights
Key Features of Taylor:
- End-to-end RCM workflow analysis to identify bottlenecks and inefficiencies
- Real-time analytics dashboards covering claims activity, collections performance, and operational KPIs
- Conversational analytics, allowing users to ask questions such as:
- How many calls did Adam AI complete last week?
- What are the most common denial reasons requiring A/R follow-up?
- How does this month’s E/M distribution compare with last month?
- Automated monthly reports highlighting hidden patterns and recommended process improvements
Best for: Hospitals, FQHCs, and large physician groups that want real-time visibility into denial patterns and RCM performance
2. CentraMed
CentraMed is a cloud-based denials analytics and workflow platform designed to help providers identify denial root causes and streamline denial management. The platform converts daily remittance data into structured denial insights, enabling billing teams to quickly understand denial trends across payers, procedures, and providers.
Along with analytics dashboards, CentraMed provides intelligent work queues and expert consulting support to help organizations reduce avoidable denials and move closer to first-pass payment.
Key Features:
- Parses 835 and 837 remittance files daily to provide a unified, up-to-date view of denials across systems.
- Automatically categorizes denials by payer, CPT code, physician, and denial code to reveal root causes.
- Creates intelligent work queues that route denied claims to billers with filing-deadline alerts.
- Provides dashboards tracking denial rate, top denial codes, backlog volume, and long-term trends.
- Includes denial strategy workshops where CentraMed experts review data and recommend operational improvements.
Best for: Hospitals, health systems, and large multi-specialty groups
3. Imagine Co-Pilot
ImagineCo-Pilot is an AI “agentic” layer built on top of the ImagineOne RCM platform that automates large portions of the claims and denial lifecycle.
It acts as a co-pilot for revenue cycle teams, using AI and NLP to correct claims before submission and resolve many denials automatically. The platform offers to reduce manual follow-up work while improving first-pass payment and overall RCM efficiency.
Key Features:
- Automates end-to-end claim workflows in ImagineOne, from claim submission to denial resolution.
- Uses AI to identify and correct claim errors before submission, helping reduce avoidable denials.
- Automatically resolves many denials with reported 95%+ accuracy, routing only exceptions to staff.
- Provides real-time reporting showing denial resolution performance and operational impact.
- Extends automation to front-end processes, including eligibility checks and patient communication.
Best for: Provider organizations already using or planning to adopt ImagineSoftware’s RCM platform
4. Rivet Health Payer Performance
Rivet Health’s Payer Performance platform focuses on identifying and recovering underpayments and payment variances rather than traditional claim denials. The platform centralizes payer contracts and analyzes claims data to detect reimbursement discrepancies, helping practices recover lost revenue and strengthen payer negotiations.
Key Features:
- Centralized contract management that stores payer agreements, tracks renewal timelines, and models proposed rate changes.
- Automated underpayment detection using AI to flag payment variances and group similar claims into prioritized recovery projects.
- Customizable worklists that allow teams to review claims, assign tasks, and export project data for payer appeals.
- Claims analytics dashboards tracking revenue performance, pricing trends, and payer behavior.
- Contract benchmarking tools that compare reimbursement rates across payers and markets to support negotiations.
Best for: Physician groups, ambulatory providers, and multi-specialty practices
5. Experian Denial Management
Experian Health’s Denial Workflow Manager is a denial management and analytics solution that helps healthcare organizations identify, prioritize, and resolve denials faster. By combining ERA data, claim status information, and customizable rules, the platform automates denial triage and follow-up while providing analytics to track root causes and improve upstream processes.
Key Features:
- Identifies and prioritizes denials using ERA data, claim status updates, holds, suspends, and zero-pay claims.
- Automatically categorizes denials with ANSI and payer-specific reason codes to speed triage.
- Provides customizable worklists based on denial category, dollar value, or client-defined rules.
- Supports root cause analysis and trend reporting to help teams prevent recurring denials.
- Integrates with Experian ClaimSource and other Experian RCM tools for a unified claims and denial workflow.
Best for: Hospitals and medical groups looking for a scalable denial workflow solution
Top Features to Look for in a Denial Management Analytics Solution
Not all denial analytics tools are built the same. Some simply show reports after denials occur, while others help organizations identify root causes, prioritize AR follow-up, and prevent future denials across the entire revenue cycle.
Here are the key capabilities to look for in an AI denial analytics platform:
Unified Denial Intelligence Across the Revenue Cycle
A strong denial analytics solution should provide a centralized view of denial performance across payers, providers, service lines, and locations. With this level of visibility, revenue cycle leaders can quickly identify where denials originate and which areas are driving the most financial impact.
Recommended Reading: Denial management in healthcare
Root Cause Analytics, Not Just Denial Reporting
Simply listing denial codes isn’t enough. Effective platforms must map denial data to operational root causes so teams can address the underlying issues.
For example, a denial analytics platform should help answer questions like:
- Are prior authorization failures increasing for a specific payer?
- Are certain CPT codes frequently denied for medical necessity?
- Is a specific provider generating a higher share of coding-related denials?
Real-Time RCM Performance Insights
The best platforms provide analytics across both operational activity and financial outcomes, helping leaders understand how workflows affect revenue performance.
For example, organizations should be able to monitor metrics such as:
- Claims submitted or processed
- Denial rates and denial backlog
- Net collection rate
- Average days in accounts receivable (A/R)
This broader view helps identify operational bottlenecks that may indirectly contribute to denials.
Conversational or Self-Service Analytics
Modern denial analytics solutions must support conversational analytics, allowing users to ask questions such as:
- What are the most common denial reasons requiring follow-up this month?
- Which payer generated the highest denial rate last quarter?
- How has our denial rate changed compared to last month?
This kind of self-service access allows operational teams to identify issues faster and take action sooner.
Automated Reporting and Pattern Detection
A strong denial analytics platform should continuously analyze claims data and surface patterns automatically.
Instead of relying on manual reporting, the system should generate:
- Monthly or weekly denial summaries
- Alerts when certain denial types spike
- Insights into recurring payer behaviors
- Recommendations for workflow improvements
Ready to Reduce Denials With AI-Powered Denial Analytics?
As denial rates continue to rise, relying on manual reviews and reactive appeals is no longer sustainable.
If you want to see how AI-driven denial analytics can uncover hidden revenue leakage and streamline your denial workflows, book a demo with CombineHealth. Our platform gives you real-time visibility into denial trends, payer behaviors, and RCM bottlenecks—so your team can focus on fixing issues at the source and getting claims paid faster.
FAQs
What is Denial Analytics?
Denial analytics refers to analyzing healthcare claim denial data to identify patterns, root causes, and operational issues that lead to denied claims. It helps revenue cycle teams understand why denials occur and implement process improvements to reduce future denials and improve reimbursement rates.
Why is Denial Analytics Important for Hospitals?
Denial analytics helps hospitals identify recurring denial patterns, reduce revenue leakage, and improve clean claim rates. By understanding payer behaviors and operational gaps, hospitals can prevent avoidable denials, reduce A/R days, and improve financial performance across the revenue cycle.
What are the Layers of Denial Analytics?
Denial analytics typically includes three layers: data aggregation (collecting denial data), pattern analysis (identifying trends by payer, provider, or service), and root cause analysis (determining operational issues causing denials). Advanced platforms also add predictive insights and workflow prioritization.
What Are the Top 10 Denials in Medical Billing?
Common denial categories include eligibility errors, missing patient information, prior authorization failures, coding errors, medical necessity denials, duplicate claims, timely filing issues, incorrect modifiers, non-covered services, and coordination of benefits errors.
How Can I Effectively Reduce Claim Denials in Medical Billing?
Reducing claim denials requires improving front-end eligibility checks, verifying prior authorizations, ensuring accurate coding, monitoring denial trends, and using analytics tools to identify root causes. Many organizations also implement claim edits and denial dashboards to catch issues before submission.
What Features Should I Look for in Healthcare Denial Management Solutions?
Look for solutions that offer denial dashboards, root cause analytics, automated denial categorization, customizable worklists, real-time reporting, payer trend analysis, and integration with EHR or billing systems. Advanced tools also provide AI-driven insights and workflow automation.
How does AI Improve Denial Analytics?
AI improves denial analytics by automatically categorizing denials, detecting patterns across large claims datasets, and identifying root causes faster than manual analysis. It helps revenue cycle teams prioritize high-impact issues, automate reporting, and uncover operational bottlenecks driving denials.
What KPIs Should Denial Analytics Track?
Key denial analytics KPIs include denial rate, first-pass claim acceptance rate, denial write-off rate, denial overturn rate, average days to resolve denials, denial dollars by payer, and clean claim rate. These metrics help organizations measure denial performance and financial impact.






