Top 10 Clinical Documentation Improvement Software Vendors for 2026
Here's our compilation of the top 10 clinical documentation improvement software vendors that can help your healthcare organization prevent claim denials and improve cash flow.
February 27, 2026
.png)

Key Takeaways:
• Poor clinical documentation is a major revenue risk. CMS estimates ~60% of improper payments are caused by insufficient documentation.
• AI-powered CDI tools help detect gaps early. They analyze charts at scale to identify missing details, unclear diagnoses, and coding opportunities.
• Modern CDI solutions combine coding, auditing, and analytics. The best tools integrate with EHRs and support proactive documentation improvement.
• Different tools serve different needs. Some focus on ambient documentation, while others specialize in chart review, compliance monitoring, or coding automation.
• Autonomous coding and AI-driven chart analysis are emerging as the most impactful capabilities for improving documentation accuracy and reducing denials.
Clinical documentation errors are one of the most common (and costly) problems in healthcare revenue cycles.
CMS reports that nearly 60% of improper payments stem from insufficient documentation, making documentation quality one of the biggest drivers of revenue leakage in healthcare. A missing diagnosis detail, unclear procedure note, or incomplete clinical evidence can easily lead to under-coding, claim denials, or compliance issues.
The challenge is that these gaps often go unnoticed until a claim is rejected or revenue is already lost.
That’s why many healthcare organizations are turning to AI-powered clinical documentation improvement software. These tools analyze patient records at scale, identify documentation gaps early, and help teams ensure that clinical documentation accurately reflects the care delivered.
In this guide, we’ll look at 10 clinical documentation improvement software vendors and how they help hospitals, physician groups, and revenue cycle teams improve documentation accuracy, reduce claim denials, and protect revenue.

Why Do You Need AI Clinical Documentation Integrity Software
Clinical documentation sits at the center of healthcare operations. Every diagnosis, treatment decision, procedure, and patient outcome must be accurately captured in the medical record. When documentation is incomplete or unclear, it doesn’t just affect the chart—it impacts coding accuracy, reimbursement, quality reporting, and even compliance with regulatory standards.
That’s why clinical documentation integrity (CDI) programs exist: to ensure medical records fully reflect the care delivered. Strong CDI practices help healthcare organizations maintain accurate coding, support clinical decision-making, and protect revenue.
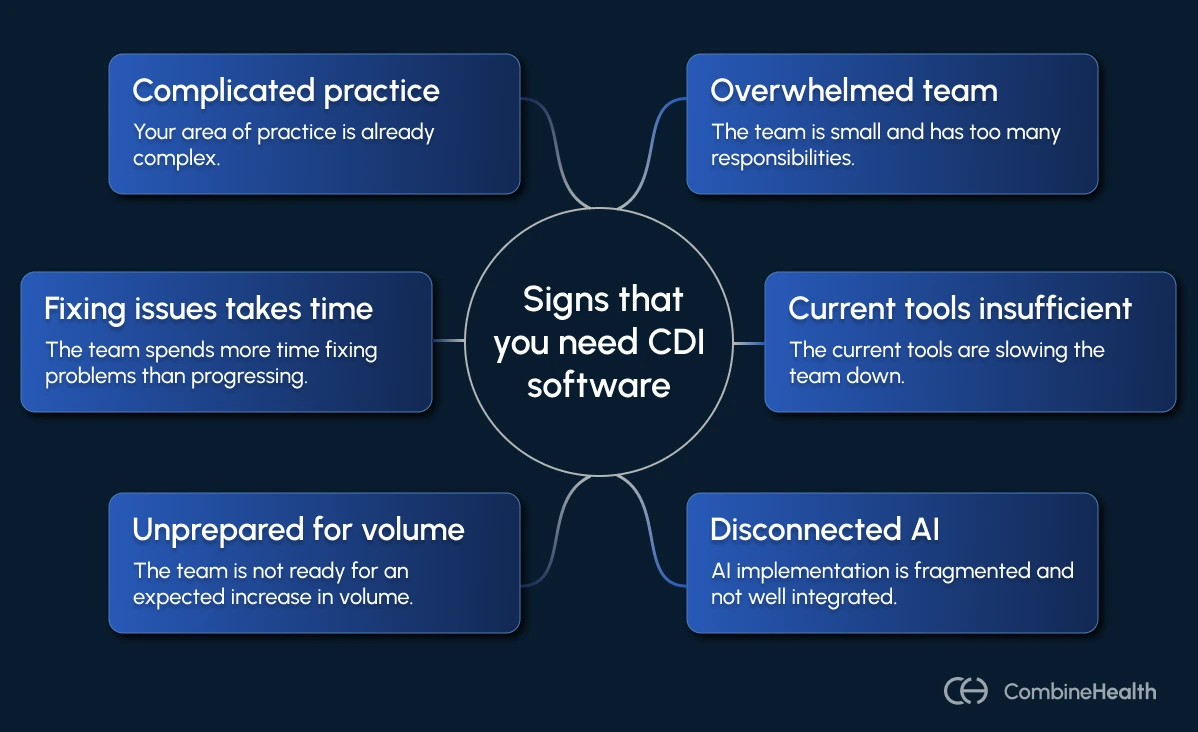
But modern healthcare documentation has become far too complex for traditional CDI workflows.
Hospitals today deal with challenges that make traditional CDI workflows difficult to scale, such as:
- Massive volumes of patient records that CDI teams cannot realistically review manually
- Constantly changing payer and regulatory requirements that affect coding and reimbursement
- Clinical data spread across multiple systems, including progress notes, labs, imaging reports, and orders
- Retrospective chart reviews that catch documentation gaps only after claims are submitted
This is where AI-powered CDI software changes the game.
Recommended Reading: Buyer’s guide for CDI software in healthcare
How Does a CDI Software Help Hospitals Improve Coding Accuracy and Reimbursement

Here’s how an AI-powered clinical documentation improvement software works:
- Detect documentation gaps early: AI can flag missing specificity, incomplete diagnoses, or unclear procedure documentation before claims are submitted.
- Improve coding accuracy and reimbursement: Better documentation leads to more accurate coding, improved DRG assignment, and more complete capture of patient complexity.
- Reduce manual chart review workload: Instead of reviewing every chart manually, CDI teams can focus on high-risk cases identified by AI.
- Lower denial and audit risk: By ensuring documentation aligns with coding guidelines and payer requirements, AI tools help reduce compliance risks.
- Support clinicians without adding extra work: Many AI CDI platforms integrate directly into EHR workflows, helping providers improve documentation without interrupting patient care.
10 Best CDI Solutions for Hospitals And Health Systems
1. CombineHealth’s Amy: Best CDI solution for Large Hospitals
Amy is CombineHealth’s autonomous AI medical coding solution that also functions as a frontline clinical documentation integrity safeguard. As she reads provider notes and assigns medical codes, she simultaneously identifies documentation gaps that could lead to under-coding, claim denials, or compliance risks.
As she works through each chart, Amy also identifies:
- Missing details
- Vague language
- Incomplete clinical evidence
Amy helps organizations strengthen documentation quality early in the revenue cycle rather than fixing issues after claims are submitted. This proactive approach enables coding teams, CDI specialists, and providers to address documentation gaps sooner, improving coding accuracy, reducing denial risk, and ensuring claims are supported by complete and defensible clinical documentation.
Key Features:
- Autonomous coding across outpatient standards, including ICD-10, CPT, HCPCS Level II, E/M levels, modifiers, and HCC capture
- Configurable coding logic with support for custom guidelines and payer-specific coding rules
- Direct analysis of encounter notes from EHR systems without manual data extraction
- Line-by-line coding rationale that shows the clinical evidence behind every coding decision
- Ability to audit pre-coded charts to identify systemic coding or documentation issues
Detection of documentation gaps such as missing procedure details, incomplete findings, or unclear interpretations
Best For: Hospitals, physician groups, and MSOs that want a unified AI solution for autonomous coding, chart auditing, and proactive CDI improvement.
2. Heidi Health
Heidi Health is an AI-powered ambient documentation platform that turns patient–clinician conversations into structured, billing-ready medical notes. Designed to reduce charting time while improving documentation accuracy, it helps teams capture more complete clinical details at the point of care.
With real-time transcription, coding support, and deep EHR integrations, Heidi Health strengthens clinical documentation workflows while supporting revenue integrity and clinician efficiency.
Key Features
- AI medical scribe that transcribes consultations in real time and generates structured, specialty-specific notes in 110+ languages
- Built-in billing and coding support with revenue-ready notes and suggested billable codes
- EHR integration with one-click export to Epic, Best Practice, MedicalDirector, and other EMR/PMS systems
- Customizable templates, clinician-specific note styles, and workflow tools for tasks, referrals, and patient handouts
Best For: Outpatient and ambulatory care teams looking to improve CDI through ambient documentation
3. EnjoinCDI
EnjoinCDI takes a different path from traditional CDI software by putting physicians at the center of documentation improvement. Instead of relying only on automation, it blends clinical education, analytics, and pre-bill validation to help organizations close documentation gaps before they impact reimbursement.
The result is a CDI approach that focuses on long-term performance—improving CMI, reducing denial risk, and helping teams align documentation with evolving value-based care expectations.
Key Features
- Physician-led chart reviews with peer-to-peer education and clinical validation
- Analytics-driven insights for CMI tracking, HCC risk adjustment, and ROI reporting
- CDocT workflow app for DRG validation and denial prevention
- Workforce support and regulatory alignment across CMS and quality initiatives
- Collaborative workflows that connect physicians, coders, and CDI teams
Best for: Mid-to-large health systems and hospital networks
4. SmarterDx SmarterPrebill
SmarterPrebill is designed for hospitals that want to catch missed documentation and coding opportunities before claims are submitted.
By reviewing the full patient record prior to billing, it helps CDI and coding teams identify diagnoses and procedures that may have been overlooked during the initial documentation process. This pre-bill approach helps organizations improve revenue capture while strengthening quality reporting tied to clinical documentation.
Key Features
- AI-driven full-chart review of inpatient discharges analyzing thousands of clinical data points
- Evidence-backed coding and documentation recommendations with supporting clinical context
- Performance dashboards that track financial and quality impact across providers and facilities
- Results-based pricing model with no upfront costs
- Rapid deployment designed to fit into existing CDI and coding workflows
Best for: Mid-to-large hospitals that want to uncover missed revenue opportunities before claims are submitted.
5. Brellium AI Chart Auditing
Brellium focuses on helping healthcare organizations maintain compliant, audit-ready documentation without adding manual review work. The platform automatically reviews patient charts to identify coding, billing, and clinical documentation issues before claims are submitted.
By combining automated auditing with provider feedback, it helps teams improve documentation quality over time while reducing the risk of denials, payer audits, and revenue clawbacks.
Key Features
- AI-powered chart auditing that reviews records against coding, billing, and compliance rules
- Automated provider feedback and coaching to improve documentation quality
- Built-in audit response tools that assemble evidence for payer reviews
- Organization-wide dashboards for compliance monitoring and documentation trends
- Seamless EMR integrations to fit into existing documentation workflows
Best for: Behavioral health organizations and outpatient practices that want automated chart auditing.
6. Adentris
Adentris helps hospitals move from reactive chart audits to real-time documentation and compliance monitoring. Instead of reviewing charts after discharge, the platform continuously scans EHR data to identify documentation gaps, safety risks, and compliance issues while care is still in progress.
This proactive approach helps CDI, quality, and compliance teams resolve problems early—reducing audit exposure, preventing revenue loss, and improving documentation accuracy across the organization.
Key Features
- AI-driven monitoring of EHR documentation against thousands of regulatory and payer rules
- Real-time alerts that surface safety risks, missing documentation, and compliance issues
- AutoFix capability that drafts EHR corrections for clinician review and approval
- Analytics dashboards for compliance tracking, root-cause analysis, and audit readiness
- Configurable monitoring for clinical protocols, quality initiatives, and regulatory requirements
Best for: Mid-to-large hospitals that want to prevent revenue-impacting errors and stay audit-ready
7. Ambience CDI
Ambience Healthcare helps health systems improve clinical documentation and coding accuracy directly during patient encounters.
By capturing conversations in real time and generating structured notes within the EHR, it reduces the documentation burden on clinicians while surfacing coding and risk-adjustment opportunities at the point of care. This approach allows organizations to strengthen CDI earlier in the workflow instead of relying on retrospective chart reviews.
Key Features
- Ambient AI documentation that captures patient encounters and generates structured clinical notes
- Built-in coding intelligence that surfaces HCC, E/M, and ICD-10 opportunities during documentation
- Native Epic integration that embeds the workflow directly into clinician documentation tools
- Compliance-focused documentation designed to reduce queries and support audit readiness
- Analytics dashboards for monitoring documentation quality, clinician adoption, and financial impact
Best for: Large health systems with high-volume specialties.
8. Layer Health
Distill by Layer Health helps health systems unlock insights from the vast amount of unstructured clinical data buried in patient charts.
Using large language models, it analyzes longitudinal patient records to identify documentation gaps, validate coding, and support CDI and quality reporting at scale. By automating complex chart review and abstraction tasks, Distill enables organizations to improve revenue integrity while reducing the manual workload placed on CDI and quality teams.
Key Features
- LLM-powered analysis of longitudinal patient records across notes, labs, imaging, and other clinical data
- Automated identification of documentation gaps and coding validation opportunities
- Configurable modules for CDI workflows, registry submissions, and quality reporting
- Seamless integration with EHR systems and existing analytics tools
- Enterprise dashboards for tracking trends, performance, and ROI
Best for: Large health systems handling massive volumes of unstructured clinical data.
9. AGS CDI
AGS Health’s Computer-Assisted CDI solution helps hospitals scale their documentation improvement programs by using AI to analyze charts and prioritize high-impact cases. Designed to support collaboration between CDI specialists, coders, and physicians, the platform surfaces documentation gaps early and enables teams to address them before coding is finalized.
This helps organizations improve documentation quality, reduce denial risk, and gain clearer visibility into the financial impact of CDI efforts.
Key Features
- AI-driven chart analysis that identifies documentation gaps and prioritizes cases with high query potential
- Real-time EHR synchronization that supports concurrent CDI and physician collaboration
- Built-in encoders, groupers, and standardized query templates to support accurate coding
- Performance dashboards tracking CMI, quality metrics, provider compliance, and CDI productivity
- Optional auditing tools that flag compliance risks and coding variances
Best for: Large hospital systems looking to scale documentation improvement across high patient volumes.
10. Evidently CDI
Evidently helps health systems make sense of the massive volumes of unstructured data scattered across clinical systems. By analyzing information from EHRs, labs, imaging, and external records, the platform builds a unified patient view that supports documentation improvement, coding accuracy, and quality reporting.
This enables CDI and revenue cycle teams to identify gaps, strengthen clinical documentation, and capture reimbursement opportunities without adding extra administrative work for clinicians.
Key Features
- AI-driven analysis that consolidates patient data from multiple clinical systems
- Automated identification of documentation gaps, HCC opportunities, and coding improvements
- Knowledge graph technology that connects medical concepts to uncover quality and revenue insights
- Workflow integrations and dashboards that track clinical, operational, and financial impact
- Customizable tools and implementation support tailored to organizational workflows
Best for: Large health systems that want actionable insights for CDI, quality reporting, and revenue optimization.
Key Features to Look For in A Healthcare CDI Solution
Not all CDI tools solve the same problems. Some focus on retrospective audits, while others support concurrent reviews or coding assistance. The most effective CDI solutions today combine automation, clinical intelligence, and coding expertise to help teams identify documentation gaps earlier in the revenue cycle.
When evaluating a CDI platform, look for the following capabilities:
- AI-driven chart analysis: A strong CDI solution should be able to read and interpret clinical documentation directly from patient records. This includes analyzing encounter notes, procedures, lab findings, and other clinical details to identify potential documentation gaps or missing diagnoses.
- Automated coding support: Modern CDI solutions often include coding intelligence that extracts diagnosis, procedure, and evaluation & management (E/M) codes directly from clinical notes.
- Documentation gap detection: One of the most important capabilities of CDI software is the ability to detect incomplete or ambiguous documentation. For example, missing procedure details, unspecified diagnoses, or incomplete clinical findings can all impact claim approval or reimbursement.
- Coding transparency and audit support: Coding decisions must be defensible during audits and payer reviews. CDI platforms should provide a clear justification for suggested codes using explainable AI, including references to the exact documentation supporting each coding decision.
Capture More Revenue With Smarter Clinical Documentation
The right healthcare CDI software can help teams catch clinical documentation gaps earlier—improving documentation accuracy, coding quality, and overall revenue integrity.
If you're exploring ways to strengthen CDI while automating medical coding and chart reviews, it’s worth seeing how modern AI solutions can fit into your workflow. Book a demo with CombineHealth to see how autonomous coding and proactive documentation checks can help your team capture every legitimate dollar.
FAQs
What is clinical documentation?
Clinical documentation is the detailed record of a patient’s medical history, diagnoses, treatments, and outcomes captured during care. Key components include:
- Provider notes
- Diagnoses
- Procedures
- Medications
- Test results.
Accurate documentation is essential for quality care, correct medical coding, reimbursement, compliance, and ensuring the patient record clearly reflects the care delivered.
What are the strategies for effective clinical documentation?
Effective clinical documentation requires capturing accurate, specific, and timely patient information. Key strategies include documenting encounters in real time, using standardized terminology, clearly supporting diagnoses with clinical evidence, and ensuring coding specificity. Regular provider education, structured templates, and CDI reviews also help reduce ambiguity and improve documentation quality.
Which clinical documentation software is most user-friendly?
The most user-friendly clinical documentation tools integrate directly with EHR systems and simplify workflows for clinicians. Solutions that offer intuitive interfaces, automated chart analysis, ambient documentation, and clear coding guidance tend to be easier for providers to adopt. Tools that reduce manual entry and provide real-time suggestions are especially valuable.
Can AI help reduce errors in medical documentation?
Yes, AI can significantly reduce errors in medical documentation by analyzing clinical notes, identifying inconsistencies, and flagging missing or unclear information. AI tools can detect documentation gaps, suggest coding improvements, and ensure diagnoses are supported by clinical evidence. This helps improve coding accuracy, reduce claim denials, and strengthen compliance.
What are the best features to look for in clinical documentation tools?
Key features to look for include AI-powered chart analysis, automated coding support, documentation gap detection, and clear coding rationale for audit readiness. Strong CDI tools should also integrate with EHR systems, support provider queries, and provide analytics that help identify recurring documentation issues and improvement opportunities.
What are the benefits of human-in-the-loop controls for AI documentation?
Human-in-the-loop controls ensure AI-generated documentation and coding suggestions are reviewed by clinicians or coders before final submission. This improves accuracy, prevents automation errors, and maintains clinical oversight. It also helps organizations build trust in AI tools while ensuring compliance with coding guidelines and regulatory standards.

.webp)




